Breathing freely is something most of us take for granted. But for people living with nasal polyps, every breath can feel like trying to inhale through a pinched straw. Add in a lost sense of smell, relentless sinus pressure, and disrupted sleep, and it becomes clear why this condition can quietly chip away at quality of life.
The tricky part is that nasal polyps tend to sneak up on individuals. They start small, cause no pain on their own, and are often mistaken for a bad allergy season or a stubborn cold. By the time someone realizes what they're dealing with, the growths may have been building for months or even years.
The good news is that treatment has genuinely improved. Whether you're exploring medical treatment for nasal polyps for the first time or wondering whether surgery is really your only option, this guide covers everything you need to know, including why biologics are reshaping how doctors manage this condition.
Struggling with chronic stuffiness and sinus pressure?
What Are Nasal Polyps?
Nasal polyps are soft, benign (noncancerous) growths that form along the lining of the nasal passages or sinuses. They look somewhat like peeled grapes or teardrops and tend to cluster near the openings to the sinuses, where drainage already tends to be sluggish.
Unlike other tissue abnormalities, nasal polyps are not tumors, and
they don't indicate cancer. But that doesn't mean they're harmless. Large or numerous polyps can block airflow, interfere with normal mucus drainage, and set the stage for recurring sinus infections.
They're more common than many people realize. Studies estimate that chronic rhinosinusitis with nasal polyps (CRSwNP) affects roughly
1 to 4 percent of the general population, though the number is likely higher when accounting for undiagnosed cases.
Common Symptoms of Nasal Polyps
One reason nasal polyps symptoms often go unrecognized is that they closely mimic other conditions. People frequently attribute the signs to allergies, a lingering cold, or simply "the way they breathe."
Common symptoms include:
- Persistent nasal congestion that doesn't respond well to decongestants
- Reduced or lost sense of smell (hyposmia or anosmia), one of the most telling signs
- A decreased sense of taste, often tied to the loss of smell
- Postnasal drip and a chronic runny nose
- Facial pressure or a feeling of fullness, especially around the cheeks and forehead
- Snoring or disrupted sleep due to blocked airways
- Recurring sinus infections
If you've had these symptoms for weeks or months and over-the-counter remedies aren't making a dent, it's worth looking deeper. Getting a proper evaluation,
including allergy testing, can help pinpoint whether allergic inflammation is driving your symptoms.
What Causes Nasal Polyps?
What causes nasal polyps isn't entirely pinned down yet, but researchers have made significant progress. The leading explanation involves chronic inflammation of the nasal and sinus lining, specifically a type called "type 2 inflammation," which involves immune cells and proteins like IL-4, IL-5, and IL-13.
Certain conditions dramatically raise your risk:
- Asthma (especially when poorly controlled; read more about our
asthma treatment services)
- Allergic rhinitis, including
environmental allergies to dust, mold, and pollen
- Aspirin-exacerbated respiratory disease (AERD), sometimes called Samter's Triad
- Cystic fibrosis
- Chronic sinusitis lasting more than 12 weeks
There's also a genetic component. Nasal polyp etiology
research shows that having a first-degree relative with nasal polyps increases your own likelihood of developing them. But genetics alone aren't destiny; environmental triggers play a real role too.
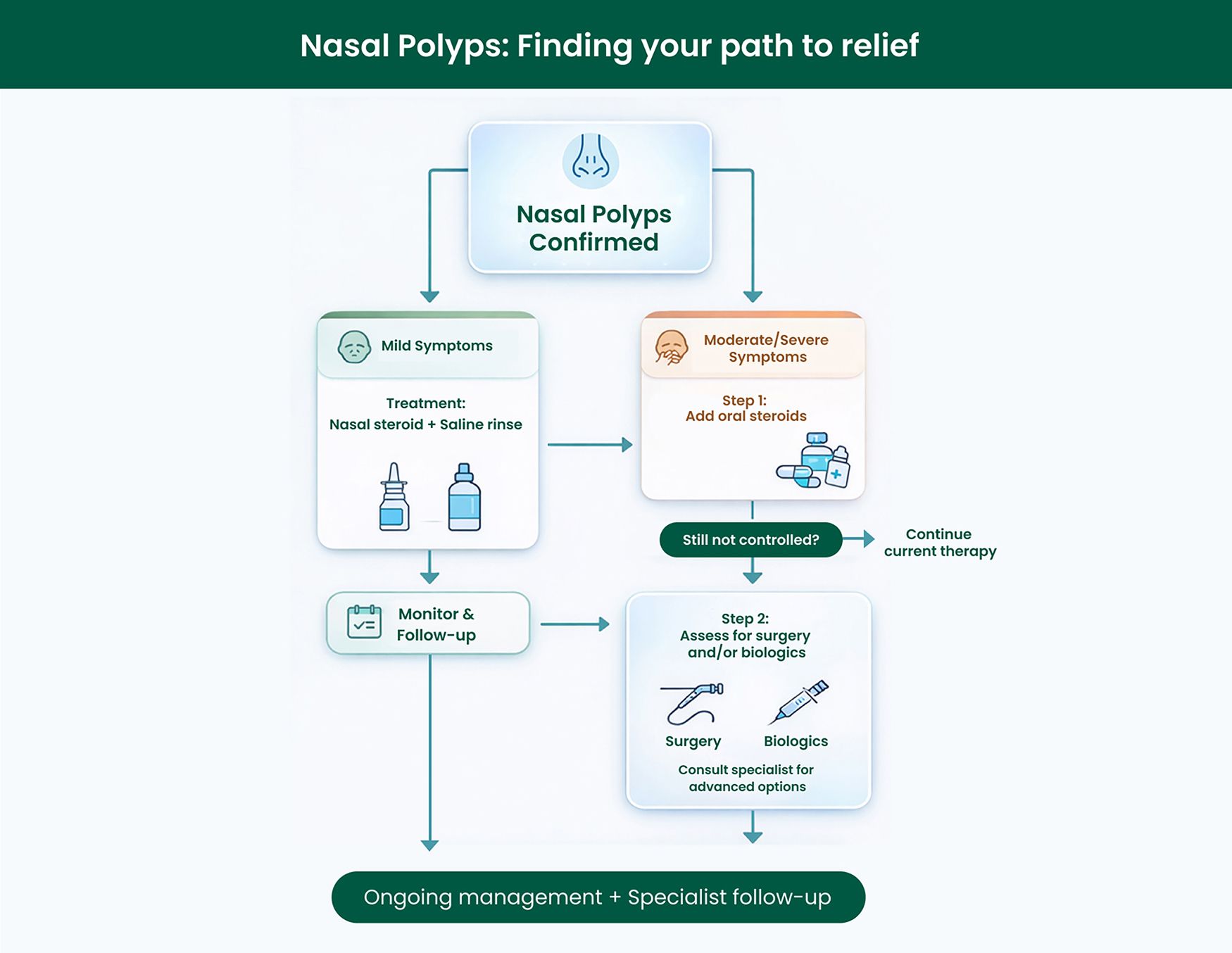
When Do Nasal Polyps Need Treatment?
For most patients, the first line of treatment for nasal polyps involves medications designed to reduce inflammation and shrink the growths.
Nasal Corticosteroid Sprays
These are the cornerstones of non-surgical management. Sprays such as fluticasone, mometasone, and budesonide reduce swelling in the nasal lining and can shrink small polyps over time. They're safe for long-term use and often the first thing a doctor recommends.
Oral or Injectable Corticosteroids
When nasal sprays aren't enough, short courses of oral steroids (like prednisone) can provide faster, more significant relief. They're effective but not ideal for long-term use due to side effects, including elevated blood sugar, loss of bone density, and immune suppression.
Saline Irrigation
Daily nasal rinses using a neti pot or squeeze bottle help flush out mucus, allergens, and inflammatory debris. While they won't shrink polyps on their own, they improve the effectiveness of other treatments and reduce the risk of infection.
Antihistamines and Allergy Management
If environmental allergies are a known trigger, managing them aggressively with antihistamines or allergen immunotherapy can reduce the inflammatory load that feeds polyp growth.
Antibiotics
Used when a bacterial sinus infection is present alongside polyps, but antibiotics don't treat the polyps themselves.
Surgery for Nasal Polyps
When medications fail to control symptoms or polyps are severely obstructing the sinuses, nasal polyps surgery becomes the next consideration.
The most common procedure is Functional Endoscopic Sinus Surgery (FESS). A surgeon inserts a thin, flexible endoscope through the nostrils (no incisions on the face) and uses small instruments to remove polyps and clear the sinus openings. Most patients go home the same day.
Surgery offers real, meaningful relief, especially for people with significantly blocked nasal passages. However, it's not a cure. Recurrence rates after surgery are high, and
studies suggest 40 to 60 percent of patients see polyps return within a few years without ongoing medical management.
Surgery works best as one part of a broader treatment plan, not a standalone solution.
Biologics Therapy for Nasal Polyps
This is where treatment has taken a genuinely exciting turn. Biologic therapy targets the specific immune pathways driving chronic inflammation in nasal polyps, rather than suppressing the entire immune system, as steroids do.
Several biologics have received FDA approval specifically for chronic rhinosinusitis with nasal polyps:
- Dupilumab
(Dupixent): Approved in 2019, it targets IL-4 and IL-13 signaling, two of the key drivers of type 2 inflammation. Clinical trials showed significant polyp shrinkage and improved nasal symptoms in patients who hadn't responded to standard treatments.
- Omalizumab
(Xolair): Approved in 2020, it targets IgE and is particularly useful for patients with allergic asthma alongside nasal polyps.
- Mepolizumab
(Nucala): Approved in 2021, it targets IL-5, reducing eosinophilic inflammation that frequently underlies severe polyp disease.
- Tezspire (Tezepelumab-ekko): Approved in 2025, it targets TSLP, a key molecule at the top of the inflammatory cascade. It has been shown to significantly reduce polyp size and nasal congestion in patients who haven't responded well to standard corticosteroids.
Biologics are typically reserved for adults with moderate-to-severe CRSwNP who haven't responded adequately to corticosteroids or surgery. They're administered as injections, usually every two to four weeks, and can be a game-changer for patients who were otherwise caught in a cycle of surgeries and steroid courses.
Patients with overlapping
immunodeficiency conditions or complex immune profiles may require additional workup before starting biologic therapy, which is another reason specialist oversight matters.
Surgery vs. Biologic Therapy for Nasal Polyps
Choosing between surgery and biologics isn't always an either/or decision; often, they complement each other. Here's how they generally compare:
For many patients with severe or recurrent polyps, the optimal path is surgical debulking followed by biologic maintenance. This combination approach reduces the inflammatory environment post-surgery and extends the time before polyps return.
Managing and Preventing Nasal Polyps Recurrence
How to cure nasal polyps permanently is a question nearly every patient asks. The honest answer is that there's currently no single intervention that guarantees polyps won't come back. But you can significantly reduce the frequency and severity of recurrence with the right ongoing strategy.
- Continuing nasal corticosteroid sprays after surgery or biologic therapy, as maintenance
- Staying consistent with saline irrigation
- Aggressively managing underlying allergies; consider whether you might benefit from allergy immunotherapy if you haven't already
- Controlling asthma well, since poorly managed asthma is one of the strongest drivers of polyp recurrence
- Avoiding aspirin and NSAIDs if you have AERD (aspirin-exacerbated respiratory disease)
- Scheduling regular follow-up appointments with your allergist or ENT to catch regrowth early
The mindset shift that helps most patients is moving from "treat when it gets bad" to "manage it consistently." Chronic conditions require a chronic strategy.
How Doctors Treat Nasal Polyps in San Antonio
San Antonio residents dealing with nasal polyps have access to a range of treatment options across allergists, ENT specialists (otolaryngologists), and immunologists. In practice, the most effective care typically involves an allergist working closely with the patient to identify and treat the inflammatory and allergic drivers of polyp growth.
An allergist brings a particular expertise that's directly relevant here. Since nasal polyp causes are so often tied to type 2 allergic inflammation, managing the whole immune picture, rather than just the physical growths, is what produces lasting results. This includes proper allergy testing to identify specific triggers, evaluating for underlying asthma, and determining whether biologic therapy is appropriate for your profile.
Finding a Specialist for Nasal Polyps Treatment in San Antonio
At Apex Allergy & Asthma, our providers take a thorough, patient-centered approach to managing nasal polyps. We understand that many patients arrive having already tried nasal sprays, rounds of antibiotics, and maybe even a prior surgery, only to find themselves back at square one. That frustration is real, and it's exactly the kind of complex case where specialist evaluation makes a genuine difference.
Our team evaluates the full clinical picture: your allergy profile, asthma status, prior treatment history, and sinus anatomy. From there, we work with you to build a treatment plan that fits your lifestyle and addresses the root cause, not just the symptoms. Whether that means optimizing your current medications, discussing biologic eligibility, or coordinating care with a surgical team, we're here to guide you every step of the way.
We serve patients at two San Antonio locations and welcome new patients ready for a more thorough approach to their nasal and allergy health.
Ready to build a long-term plan for your nasal health?
Frequently Asked Questions
What are nasal polyps, and are they cancerous?
Nasal polyps are soft, noncancerous growths on the lining of the nasal passages or sinuses. They develop in response to chronic inflammation and are not a sign of cancer, though they do require treatment when they grow large enough to affect breathing or smell.
Can nasal polyps go away without treatment?
Small polyps occasionally reduce in size when the underlying inflammation is controlled, but they rarely disappear completely without active treatment. Most polyps require medications or procedures to manage them long-term.
Who is a good candidate for biologic therapy?
Biologics are generally considered for adults with moderate-to-severe chronic rhinosinusitis with nasal polyps who have not responded adequately to corticosteroids or who continue to experience recurrence after surgery. Your allergist can evaluate whether you meet the clinical criteria for these treatments.
How do I know if my nasal symptoms are from polyps or just allergies?
The two often coexist, which makes differentiation tricky. Symptoms like a persistent loss of smell, thick postnasal drip, and congestion that doesn't respond to antihistamines are more suggestive of polyps than allergies alone. A physical exam, nasal endoscopy, or imaging can confirm the diagnosis.